Table of Contents
Kyrle Disease
Kyrle disease first defined Kyrle’s disease in 1916 as “Penetrating follicular and follicular hyperkeratosis of the body” and identified as perforating disease. To this day, controversy persists over the classification of Carrel’s disease: is it a distinct disease entity, part of the spectrum of acquired bursting dermatosis, or a subtype of acquired perforating collagenosis?
The two primary perforating diseases are reactive perforating collagenosis and perforating elastosis serpiginous. In some literature, acquired perforating dermatoses is a third major group and is a general term for adult-onset cases of perforating disease, usually associated with systemic infection.
Kyrle’s disease is characterised by the formation of large plugged papules on the central border and is often associated with liver, kidney, or diabetic disorders. It can affect men and women throughout life, although the average age of presentation is 30 years.
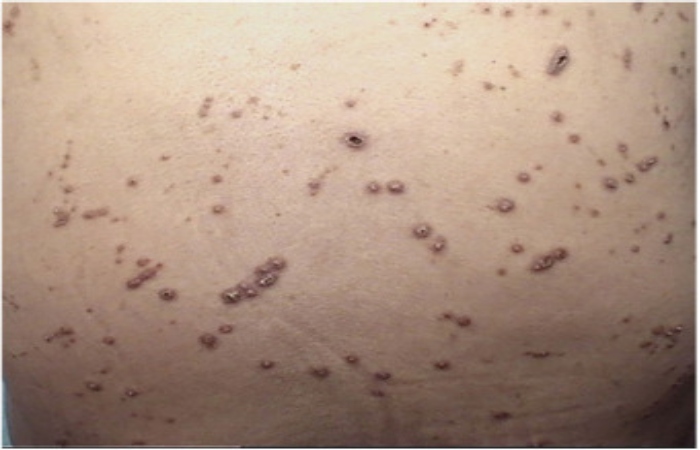
What Causes Kyrle Disease?
The cause of the disease is unknown. Some cases appear to be idiopathic (without a known trigger) or hereditary. What has been originating is that curl disease occurs more frequently in patients with certain systemic disorders, including:
- Diabetes Mellitus
- Renal disease (chronic renal failure, albuminuria, elevated blood serum creatinine, abnormal creatinine clearance, polyuria)
- Liver abnormalities (alcoholic cirrhosis)
- Congestive heart failure
What are the Signs and Symptoms?
The injuries begin as small, silvery rough papules that grow to about 1.5 cm in diameter and become reddish-brown nodules with a central plug of keratin (cornea). Multiple lesions may coalesce to form large keratotic plaques. Injuries mainly occur in the legs, arms, head, and neck regions. The palms of the hands and fillet of the sole of the feet are rarely affected. Without treatment, the lesions heal independently, but new ones continue to form. The Injuries are not painful, but patients may experience severe pruritus (itching).
How was the Diagnosis Made?
Papules or nodules are characteristic of many other central keratotic crusting and plugging disorders. Deep penetration, size and irregularity of keratotic pinnae, age of appearance, and distribution of lesions should aid in the diagnosis. It is also essential to evaluate and rule out underlying conditions such as diabetes and liver and kidney disease.
The diagnosis is confirmes by histopathology of a skin biopsy, which shows incomplete keratinisation and a hyperkeratotic parakeratotic plug.
What Treatment is Available?
Treatment should aim to treat the underlying disease if associated. Once the underlying condition treats, rapid improvement and resolution of injuries detect.
Injuries may heal independently without treatment, but new lesions often develop. Medicines used to treat and reduce scarring include:
- isotretinoin
- High intake of vitamin A
- tretinoin cream
Differential Diagnosis
Kyrle disease must distinguish from other disorders that cause a papular or nodular rash with a hyperkeratotic central plug. These include the following:
- Prurigo nodularis (some authors say that Kyrle’s disease is a variant of prurigo nodularis)
- Multiple keratoacanthomas (can mimic Kyrle disease histologically)
- Excitatory lesions (prurigo simplex)
- folliculitis
- Hypersensitivity reactions to arthropods
- Perforation of exogenous or endogenous distant material
- dermatofibromas
If koebnerization occurs, more linearly spread, lesions include in the difference. These include the following:
- Psoriasis
- lichen planus
- warts
Diagnosis can be difficult because patients with acquired perforating disorders often have concomitant folliculitis and prurigo nodule. Furthermore, histology can represent different lesions at different stages. Patients with a history of diabetes mellitus and patients with kidney disease or hemodialysis patients are more likely to develop perforation defects.
History and Physics
Curl disease typically presents as hyperkeratotic papules and nodules with a central keratotic plug. Skin lesions occur more frequently on the lower extremities, particularly the calf, tibial region, and posterior aspect. It can also affect the arms, head, and neck areas. Rarely the palms and soles are involved. Koebnerization, in which skin lesions form at injury sites, has also been reported.
Also Read: How to Lose Belly Fat?

